Pancreatic Cancer, Childhood
Introduction
Pancreatic cancer is the fourth leading cause of death among both men and women, comprising 6% of all cancer-related deaths. The incidence of pancreatic cancer has risen slowly over the years. The disease is notoriously difficult to diagnose in its early stages. At the time of diagnosis, 52% of all patients have distant disease and 26% have regional spread. The relative 1-year survival is only 24% and the overall 5-year survival rate for this disease is less than 5%.
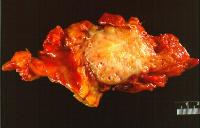
Pancreatic cancer. Gross section of an adenocarci... Pancreatic cancer. Gross section of an adenocarcinoma of the pancreas measuring 5 X 6 cm resected from the pancreatic body and tail. Although the tumor was considered to have been fully resected and had not spread to any nodes, the patient died of recurrent cancer within 1 year.
Pathophysiology
Pancreatic cancers can arise from both the exocrine and endocrine portions of the pancreas. Of pancreatic tumors, 95% develop from the exocrine portion of the pancreas, including the ductal epithelium, acinar cells, connective tissue, and lymphatic tissue. Approximately 75% of all pancreatic carcinomas occur within the head or neck of the pancreas, 15-20% occur in the body of the pancreas, and 5-10% occur in the tail.
Typically, pancreatic cancer first metastasizes to regional lymph nodes, then to the liver, and, less commonly, to the lungs. It can also directly invade surrounding visceral organs such as the duodenum, stomach, and colon or metastasize to any surface in the abdominal cavity via peritoneal spread. Ascites may result, and this has an ominous prognosis. Pancreatic cancer may spread to the skin as painful nodular metastases. Pancreatic cancer uncommonly metastasizes to bone. It is rare for pancreatic cancer to spread to the brain. It can, however, produce meningeal carcinomatosis.
The molecular genetics of pancreatic adenocarcinoma have been well studied Of these tumors, 80-95% have mutations in the KRAS2 gene, and 85-98% have mutations, deletions, or hypermethylation in the CDKN2 gene. Of these cancers, 50% have mutations in p53 and about 55% have homozygous deletions or mutations of Smad4. Some of these mutations can also be found in high-risk precursors of pancreatic cancer. For example, in chronic pancreatitis, 30% of patients have detectable mutations in p16 and 10% have K-ras mutations.
Families with BRCA-2 mutations, which are associated with a high risk of breast cancer, also have an excess of pancreatic cancer.Assaying pancreatic juice for the genetic mutations associated with pancreatic adenocarcinoma is invasive but may be useful for the early diagnosis of the disease;this approach is problematic as genetic mutations in the pancreatic juice may be found associated with inflammatory pancreatic disease.
Certain precursor lesions have been associated with pancreatic tumors arising from the ductal epithelium of the pancreas. The main morphologic form associated with ductal adenocarcinoma of the pancreas has been pancreatic intraepithelial neoplasia or PIN. These lesions arise from specific genetic mutations and cellular alterations that all contribute to the development of invasive ductal adenocarcinoma. The initial alterations appear to be related to KRAS2 gene mutations and telomere shortening. Thereafter p16/CDKN2A is inactivated. Finally, the inactivation of TP53 and MAD4/DPC4 occur. These mutations have been correlated with increasing development of dysplasia, and thus the development of ductal carcinoma of the exocrine pancreas.
As in other organs, chronic inflammation appears to be a predisposing factor in the development of pancreatic cancer. Patients with chronic pancreatitis from alcohol and especially those with familial chronic pancreatitis have much higher incidence and an earlier age of onset of pancreatic carcinoma.
Frequency United States
In 2008, an estimated 37,680 new cases of pancreatic cancer (18,770 in men and 18,910 in women) will have been diagnosed in the United States; 34,290 persons (17,500 men and 16,790 women) will have died of the disease in 2008.
The overall incidence of pancreatic cancer is approximately 8-10 cases per 100,000 persons per year Although the overall incidence of pancreatic cancer has been relatively stable for decades, the incidence of pancreatic cancer in males has been slowly dropping over the past 2 decades, while the incidence in females has increased slightly. These trends probably represent the effect of changing smoking rates for men and women.
International
Worldwide, pancreatic cancer ranks 13th in incidence but 8th as a cause of cancer death.The highest incidence rate is approximately 13 cases per 100,000 persons per year in black males in the United States. Native Hawaiian males and men of Korean, Czech, Latvian, and New Zealand Maori ancestry also have high incidence rates, that is, 11 cases per 100,000 persons per year. Most other countries have incidence rates of 8-12 cases per 100,000 persons per year. In some areas of the world, pancreatic cancer is quite infrequent; for example, the incidence in India is less than 2 cases per 100,000 persons per year.
Mortality/Morbidity
Pancreatic cancer is the fourth leading cause of death among both men and women, comprising 6% of all cancer-related deaths. The incidence of pancreatic cancer has risen slowly over the years. The death rate has risen from 5 per 100,000 population in 1930 to more than 10 per 100,000 in 2003. The disease is notoriously difficult to diagnose in its early stages. At the time of diagnosis, 52% of all patients have distant disease and 26% have regional spread.
The relative 1-year survival is only 24%, and the overall 5-year survival rate for this disease is less than 5%. This number has not changed significantly over the years. A 5-year survival in pancreatic cancer is no guarantee of cure; patients who survive for 5 years after successful surgery may still die of recurrent disease years after the 5-year survival point. The occasional patient with metastatic disease or locally advanced disease who survives beyond 2-3 years may die of complications of local spread, such as bleeding esophageal varices.
Pancreatic carcinoma is unfortunately usually a fatal disease. The collective median survival time of all patients is 4-6 months. Most patients eventually succumb to the consequences of local invasion and metastatic cancer, and true long-term cures are rare. However, neuroendocrine and cystic neoplasms of the pancreas such as mucinous cystadenocarcinomas or intraductal papillary mucinous neoplasms (IPMN) have much better survival rates than pancreatic adenocarcinoma.
In patients able to undergo a successful curative resection (only about 20% of patients), median survival time ranges from 12-19 months, and the 5-year survival rate is 15-20%. The best predictors of long-term survival after surgery are a tumor diameter of less than 3 cm, no nodal involvement, negative resection margins, and diploid tumor DNA content.





































