Adrenocortical Carcinoma Adult
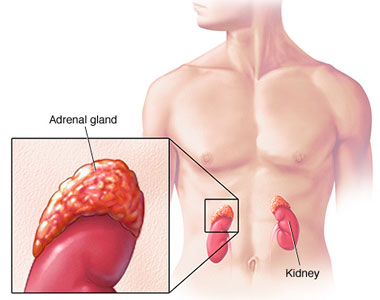 Adrenocortical carcinoma, also adrenal cortical carcinoma (ACC) and adrenal cortex cancer, is an aggressive cancer originating in the cortex (steroid hormone-producing tissue) of the adrenal gland. Adrenocortical carcinoma is a rare tumor, with incidence of 1-2 per million population annually. Adrenocortical carcinoma has a bimodal distribution by age, with cases clustering in children under 6, and in adults 30-40 years old. Adenocortical carcinoma is remarkable for the many hormonal syndromes which can occur in patients with steroid hormone-producing ("functional") tumors, including Cushing's syndrome, Conn syndrome, virilization, and feminization. Adrenocortical carcinoma has often invaded nearby tissues or metastasized to distant organs at the time of diagnosis, and the overall 5-year survival rate is only 20-35%.
Adrenocortical carcinoma, also adrenal cortical carcinoma (ACC) and adrenal cortex cancer, is an aggressive cancer originating in the cortex (steroid hormone-producing tissue) of the adrenal gland. Adrenocortical carcinoma is a rare tumor, with incidence of 1-2 per million population annually. Adrenocortical carcinoma has a bimodal distribution by age, with cases clustering in children under 6, and in adults 30-40 years old. Adenocortical carcinoma is remarkable for the many hormonal syndromes which can occur in patients with steroid hormone-producing ("functional") tumors, including Cushing's syndrome, Conn syndrome, virilization, and feminization. Adrenocortical carcinoma has often invaded nearby tissues or metastasized to distant organs at the time of diagnosis, and the overall 5-year survival rate is only 20-35%.
Hormonal syndromes should be confirmed with laboratory testing. Laboratory findings in Cushing syndrome include increased serum glucose (blood sugar) and increased urine cortisol. Adrenal virilism is confirmed by the finding of an excess of serum androstenedione and dehydroepiandrosterone. Findings in Conn syndrome include low serum potassium, low plasma renin activity, and high serum aldosterone. Feminization is confirmed with the finding of excess serum estrogen
RadiologyRadiological studies of the abdomen, such as CT scans and magnetic resonance imaging are useful for identifying the site of the tumor, differentiating it from other diseases, such as adrenocortical adenoma, and determining the extent of invasion of the tumor into surrounding organs and tissues. CT scans of the chest and bone scans are routinely performed to look for metastases to the lungs and bones respectively. These studies are critical in determining whether or not the tumor can be surgically removed, the only potential cure at this time.
PathologyAdrenal tumors are often not biopsied prior to surgery, so diagnosis is confirmed on examination of the surgical specimen by a pathologist. Grossly, adrenocortical carcinomas are often large, with a tan-yellow cut surface, and areas of hemorrhage and necrosis. On microscopic examination, the tumor usually displays sheets of atypical cells with some resemblance to the cells of the normal adrenal cortex. The presence of invasion and mitotic activity help differentiate small cancers from adrenocortical adenomas.There are several relatively rare variants of adrenal cortical carcinoma: Oncocytic adrenal cortical carcinoma, Myxoid adrenal cortical carcinoma, Carcinosarcoma, Adenosquamous adrenocortical carcinoma, Clear cell adrenal cortical carcinoma. Differential diagnosis includes: Adrenocortical adenoma, Renal cell carcinoma, Adrenal medullary tumors, Hepatocellular carcinoma.
TreatmentThe only curative treatment is complete surgical excision of the tumor, which can be performed even in the case of invasion into large blood vessels, such as the renal vein or inferior vena cava. The 5-year survival rate after successful surgery is 50-60%, but unfortunately, a large percentage of patients are not surgical candidates. Radiation therapy and radiofrequency ablation may be used for palliation in patients who are not surgical candidates.
Chemotherapy regimens typically include the drug mitotane, an inhibitor of steroid synthesis which is toxic to cells of the adrenal cortical as well as standard cytotoxic drugs. A retrospective analysis showed a survival benefit for mitotane in addition to surgery when compared to surgery alone. One widely used regimen consists of cisplatin, doxorubicin, etoposide) and mitotane. The endocrine cell toxin streptozotocin has also been included in some treatment protocols. Chemotherapy may be given to patients with unresectable disease, to shrink the tumor prior to surgery (neoadjuvant chemotherapy), or in an attempt to eliminate microscopic residual disease after surgery (adjuvant chemotherapy). Hormonal therapy with steroid synthesis inhibitors such as aminoglutethimide may be used in a palliative manner to reduce the symptoms of hormonal syndromes.
Further Inpatient Care- Patients with adrenal carcinomas who undergo complete surgical resection with no evidence of continuing functional hormone production do not require further inpatient care.
- If the patient has evidence of local or distant metastases during ambulatory follow-up, aggressive attempts at repeat resection should be undertaken. These attempts lead to additional inpatient care.
- If treatment includes intensive chemotherapy, further inpatient care is necessary to deliver chemotherapy or to treat chemotherapy-related toxicity.
- If lesions seem particularly sensitive to chemotherapy, with dramatic diminishment of tumoral masses in the chest or elsewhere, autologous transplantation might be a consideration. However, only anecdotal data suggest that transplantation is helpful in managing this disease. One study reported the use of chemotherapy, surgical debulking of lung metastases, and autologous transplantation; 2 years of continuous complete remission was reported.
- Ambulatory follow-up should occur every month for the first 2 years after treatment because repeat resection of locally recurring disease and resection of metastatic lung disease can substantially affect long-term survival.
- Scanning of the local area in the abdomen or pelvis and of sites of metastatic disease should continue every 3 months for the first 2 years, every 4 months for the next 2 years, and every 6 months during the fifth year.
- Patients should be monitored for the reappearance of adrenocortical hormone hyperactivity, along with scanning, unless their history suggests that Cushing syndrome or autonomous adrenocortical hormonal production is present. If this is the case, the physician should immediately search for recurrence.





































